The coronavirus has invaded the world. Hospitals are overwhelmed and there is a major shortage of medical equipment. All over the world, doctors, nurses and other healthcare staff are working tirelessly to treat the sick and combat the virus.
If wealthy countries like Spain, Italy and Belgium are struggling, imagine what it will be like when the virus spreads to the poorest regions. Military occupation, lack of access to drinking water, substandard housing - all these factors make the fight against the virus an extremely difficult ordeal.
Added to this is the fact that many countries have very weak health systems. Under pressure from the World Bank and the International Monetary Fund, developing countries have made drastic cuts in healthcare. The health system has often fallen into the hands of the private sector and is in the process of collapse in many countries.
On 3 April, Dr Tedros Adhanom Ghebreyesus, Director of the World Health Organisation, gave member countries three pieces of advice for overcoming the coronavirus crisis. Firstly, they need to invest in public health and not just in medical interventions. Secondly, member countries need to strengthen the foundations of their healthcare systems by paying medical staff properly and funding medical infrastructure and equipment. Finally, there must be no more financial barriers for the most vulnerable groups.
It is clear that he is arguing for strong public healthcare. This is also a prerequisite for beating the coronavirus. And here's why.
1. Public healthcare is accessible to all
This is not the case in countries where healthcare is provided by private companies. Their primary aim is to make money, so priority is given to the richest patients.
This creates a two-tier system. One offers highly specialised care for those who can afford it, while the other, because of a lack of resources, is unable to offer even the most basic care. Such a system, in which access to care depends on the price of a treatment or drug, makes it impossible to tackle the coronavirus effectively.
In the United States, for example, 30 million Americans have no health insurance. If they are absent from work because of illness, they lose their salary. If they have to undergo a test or treatment, they have to pay for it themselves. This means that many Americans have to make a choice: save money or get treatment, at any time of the year, and not just in the current climate. As a result, the United States runs the risk of a constant spread of the virus.
Public health care, on the other hand, is aimed at the whole population, not just those who can afford it. It ensures that everyone is protected and healthy. Whether you're rich or poor, male or female, black or white - it doesn't matter. In principle, everyone has access to healthcare, medicines and vaccines.
In the case of an epidemic like the coronavirus, this is obviously essential. Protection is only as strong as the weakest link. And we are only well protected when everyone is protected. It is therefore essential that everyone has access to healthcare.
2. Public healthcare invests in prevention
According to the World Health Organisation, one of the most important lessons about containing the virus comes from China and other East Asian countries. There is massive investment in prevention. The last contacts of infected people are meticulously recorded, traced and discarded in the event of a positive test. This eases the pressure on hospitals and means that not everything rests entirely on the shoulders of doctors and nurses.
Stopping the spread of the virus therefore requires more than medical staff and the right equipment. You have to act to prevent it. And that's something that's very important in a public healthcare system. Such a system tackles health problems at source and invests heavily in prevention and care in the broadest sense. Unless, as in Belgium, there are no effective preventive structures. In that case, it's mainly in the hospitals that the fight against the virus takes place.
Now that the virus has appeared in Palestine, Congo and the Philippines, our partners are springing into action. In the Congo, Etoile du Sud is doing everything possible to prevent a conflagration. Thanks to their experience in the fight against Ebola, they know how to get organised. They mobilise health activists, prepare local branches via social media and send out clear prevention messages. They go door-to-door to raise people's awareness and inform them of the essential measures to be taken.

In Palestine, the occupation by the Israeli army is causing enormous difficulties. If the virus were to spread to the Gaza Strip, which is completely cut off from the outside world, it would be a catastrophe for the population. As a result of the Israeli blockade and invasions, there are not enough intensive care beds, respirators, medicines or trained staff to deal with this crisis. This is why they are doing everything they can to keep the number of cases as low as possible.
For fear that hospitals and medical centres would be unable to cope with a major spread, our partners are concentrating their efforts on containing the virus by preventive means. The current situation compels them to do so. Of course, they are continuing their fight for strong public healthcare and better living conditions for the population. They are urging the authorities to take responsibility and make choices to prevent people from becoming infected.
3. A public health system guarantees rational investment of resources
On 11 March, Dr Tedros, Director of the World Health Organisation, sent the following message to governments: «Countries can still change the course of this pandemic if they take a proactive approach to detecting, testing, treating, isolating, tracking and mobilising the population».
As long as there is no vaccine, the fight against the coronavirus can only be won with a wide-ranging approach that goes well beyond the medical aspect alone.
We need public healthcare to facilitate coordination. It strengthens cooperation, making it more efficient and faster. If we prepare hospitals and medical staff in the same way for a wave of contamination, we can react much better. We can also quickly exchange equipment, medicines and hygiene products. Hospitals in less infected regions can quickly send equipment to where it is most needed.
What's more, a strong public healthcare system is closer to the people. This direct link with citizens is very important, especially in a health crisis such as this. Vital information needs to be passed on quickly. And good monitoring by doctors in the local healthcare system means that sick people can be detected, treated and cared for quickly. Cuba is a model in this respect. Despite the US blockade, Cuba has one of the best healthcare systems in the world. The United States is eight times richer than Cuba, yet its infant mortality rate is higher. The number of cases of coronavirus in Cuba at the beginning of April remains low.
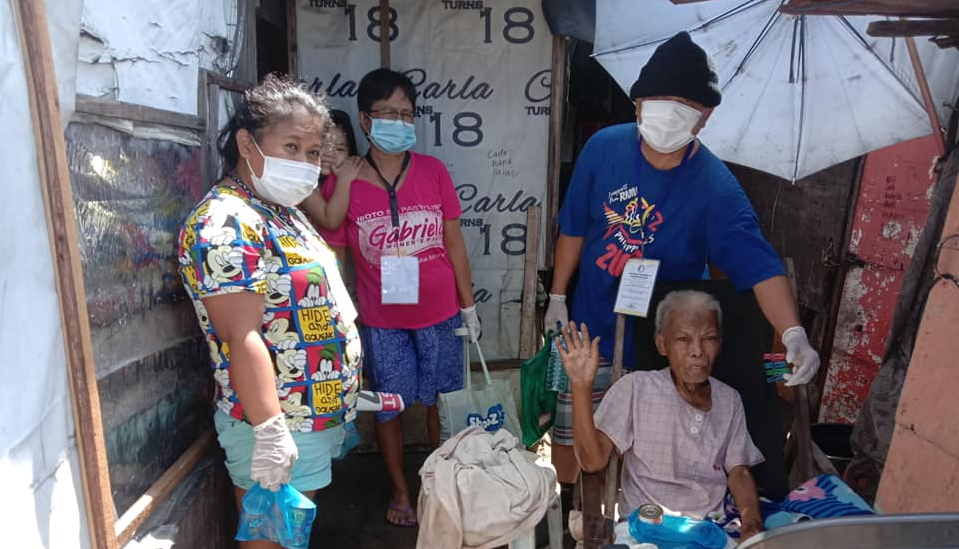
On the other hand, countries where healthcare is in private hands are unable to respond effectively to the crisis. The healthcare system there is like a patchwork of hundreds of systems with their own conditions, rules and characteristics. This makes cooperation virtually impossible. Some countries are adopting a hard-line policy, basing their approach primarily on isolating the population. For example, Gabriela, one of our partners in the Philippines, warns against the disastrous measures taken by President Duterte. He has declared a state of emergency for 6 months and has sent the army and police into the streets to check that the population is complying with the quarantine. These measures are a disaster for the millions of poor families who have no income and cannot protect themselves from the virus because they lack access to water and decent housing.
It is therefore absolutely vital that we continue to support our partners in the Congo, Palestine and the Philippines. More than ever, international solidarity is needed and we must continue the fight for strong public healthcare. Everywhere.




